Recently, the American Academy of Pediatrics (AAP) released a report written by Dr. Mary Ott and Dr. Gina Sucato and the COMMITTEE ON ADOLESCENCE indicating intrauterine devices (IUD’s) and implants are the best method of birth control for adolescent women. I was already familiar with this concept; I’d attended a conference a year or so ago in which school-based health center clinicians touted this as the best option for sexually-active young women. At that time, I remember thinking…what’s wrong with the pill??? But I’ll get back to this in a minute.
Of course the BEST and ONLY way to prevent STI’s and pregnancy is abstinence. However, about half of all high school students have had sex by the time they graduate, so it is important to address topics such as contraception.
In fact, conversations about sexuality health should begin when kids are little. No, they don’t need to know about intercourse at age 4. Rather, conversations about healthy relationships, learning to assert themselves, and respecting themselves and others can be woven into everyday conversation. And remember, whether you are a parent, family member, teacher…whomever…they are watching you, so model what you preach.
But I digress
So, let’s assume you’ve had “the talk” (about relationships, I mean) and feel confident she has been taught well. But now you have been informed she would like to visit the doctor for birth control. If you start to sweat, shake, stutter, and your eyeballs fall out, explain to her that you would like to have this conversation when you have a minute to sit and chat with her. After sipping (okay, gulping) a little wine and feel a little more relaxed and ready to LISTEN, it is time to have an intelligent conversation with her.
Understanding the basics of birth control options for young women is the first step in engaging in this type of conversation. If you don’t know what options are available, it will be difficult to sound intelligent…and we don’t want them to think we don’t know what we are talking about, do we???[/vc_column_text]
Well, nothing really. At least not when it is used correctly and consistently. And that, my friend, is the problem. With perfect use, the pill is about 99% effective. However, it is rare that the pill is used perfectly. Therefore, with typical use (yes, that’s a term), the pill is about 91% effective. Not bad – unless you are the nine in 100 who become pregnant.
You are probably wondering how a pill can be used incorrectly or inconsistently. Well, here are some glitches:
- It is not taken at the exact same time every day. (Setting an alarm can help.)
- Forgetting a pill here and there. (The pill must be taken 7 consecutive days to be effective. If you miss more than one, you must use a back-up method)
- Taking a medication which may lessen the effectiveness of the pill, therefore a back-up method should be used. (Tell your healthcare provider about all medications being taken.)
- Not refilling the prescription on time each month.
According to Dr. Ott and colleagues, the oral contraceptive pill is the most commonly used method of hormonal contraception among adolescents. The pill is also an effective way to treat other reproductive health ailments, not just for prevention of pregnancy.
(Planned Parenthood)
Both the IUD and the implant (which are referred to as long-acting reversible contraception – LARC), are placed into the body for between 3-12 years, depending on the device, with nary a thought!
Implants:
The progestin implant (Implanon and Nexplanon are two commonly used) is surgically inserted into the inside of the upper arm by a specially-trained healthcare provider. It’s a quick procedure – about five minutes. It can be left in for up to three years.
(Planned Parenthood)
The IUD
IUD’s are used commonly used world-wide; we are finally catching on to this effective method in the U.S. One type of IUD contains copper which prevents pregnancy by stopping sperm in its tracks. (They don’t like copper.) This IUD can stay in the uterus about 10-12 years.
The other type of IUD contains levonorgestrel (a hormone) and also prevents sperm from making a “run for it” by causing the cervical mucus to become really thick and sticky. This type of IUD can stay in place up to 5 years, depending on the particular IUD selected.
(Planned Parenthood)
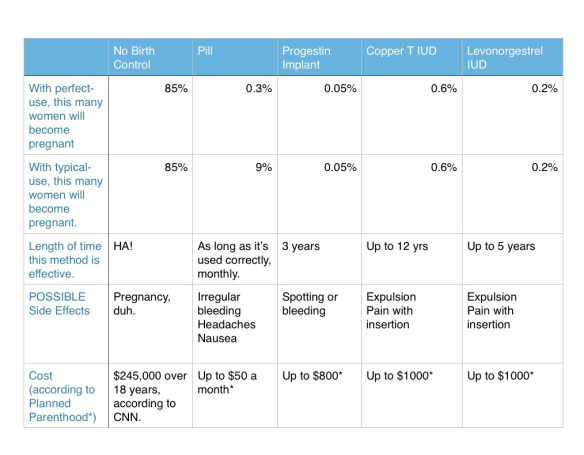
Here’s a comparison chart with information gathered by Dr. Mary Ott and Dr. Gina Sucato, CNN, and Planned Parenthood. (Okay, there are a few stray comments interjected by yours truly…)
These stats reflect the odds of pregnancy when using the specified method for one year.
Don’t get me wrong.
There IS a risk for every type of contraception. This is where a CONVERSATION WITH YOUR HEALTHCARE PROVIDER is mandatory. Information you read here, online, in books, or discussed with friends is always helpful, but we don’t know YOU or your CHILD. Your physician will offer personalized care that cannot be provided anywhere else. Information given on this site (and others) is merely to inform and get the conversation started. Keep in mind that by denying a sexually-active adolescent access to birth control, an unplanned pregnancy may become a reality.
One last word.
Having said all this, it is important to understand that hormonal methods of contraception DO NOT protect against STI’s. This is where conversation with penis-owners and vagina-owners becomes imperative. Even with the use of hormonal contraception, no matter which method works for your family member, a condom must be used in tandem to prevent the spread of STI’s and HIV. In other words, sexual health responsibility does NOT lie solely with the young woman, it is a dual responsibility. After all, it does take two to tangle, does it not? Both parties should be taught to be equally responsible for the health and well-being of not only themselves, but of their partner (that’s that “respect” topic mentioned earlier). And in the case of same-sex relationships where pregnancy is not an issue, a barrier method of birth control is recommended – not to control birth, but to help both partners stay healthy.
A special thank you to Dreyer Medical Group Obstetrician and Gynecologist Dr. Caroline Mills, MD for reviewing this post. You rock!